Early training
Descended from a long line of field naturalists, James Frederic (Jim) Riley was born in Settle, Yorkshire, in 1912. It seemed to him almost as if from that day that he had wanted to be a doctor, in particular a combination of clinician, scientist and research worker. In due course he graduated with Honours from the University of Edinburgh in 1935.
A posting as assistant surgeon to Gleneagles, a hotel that had been requisitioned as a hospital during the war, followed acquisition of the Edinburgh surgical fellowship. This was succeeded by a stint at Bridge of Earn, one of the seven Emergency Medical Service hospitals that were rapidly erected in rural Scotland in the early part of the Second World War. Later came D-Day call up to the Royal Army Medical Corps as a Lieutenant in South Wales. Subsequently, he travelled to the Far East where he commanded a mobile surgical unit, with promotion to Major.
Riley’s last posting of the War was to Malaya, where the climate of the country took its toll on his skin, with humidity rather than temperature doing the damage. Continual sweating, ‘prickly heat’ and skin fold inflammation were compounded by running out of dry surgical gloves, so that he was operating with wet gloves sterilised in weak antiseptic. His hands subsequently deteriorated with infection spreading under three of the nails, which he decided to remove and apply penicillin powder that had just become available. Scrubbing up was now out of the question. The officer in charge of postings took one look at his hands and issued a railway warrant to see the skin specialist in Singapore, and in due course came a ticket for home. However, his hands showed little sign of healing, and since the official verdict was ‘no surgery for at least a year’, he took the course for the Diploma in Medical Radiotherapy.
During those days of indecision about his future, Dr Cameron Swanson, a radiologist at Dundee Royal Infirmary (DRI), approached Riley, saying that he wished to concentrate on the therapy side of X-rays and that there would soon be a place in the department for an assistant. Riley duly applied for the post and was accepted, Dr Swanson obligingly adding a clause into the contract to enable him ‘to undertake such research work as does not interfere with his other duties’. This research work came to be conducted in the room at DRI that he shared with Dr Swanson, Riley fitting up a bench and shelf in a dark corner where he kept all the chemical dyes and reagents that he had brought from Edinburgh (Figure 1).
Figure 1 Research in a modest laboratory at Dundee Royal Infirmary

Mast cells – early days
It was Friedrich von Recklinghausen who first observed granular cells in frog mesenteries in 1863.1 Twelve years later, anatomist Wilhelm Waldeyer detected a heterogeneous group of cells in a tissue spread of rat dura mater, and named these as ‘embryonal’ or ‘plasma’ granular cells.2 In 1878, Waldeyer’s student Paul Ehrlich noted that certain cells in connective tissue contained granules with a ‘specific affinity’ for basic dyes, such as methylene blue, which had been synthesised the year before. As many of these cells were present in areas of lymph stasis or enhanced nutrition, such as that in chronic inflammation or around tumours, Ehrlich named these cells Mast-zellen, since the histological appearances suggested to him that they were well-fed cells that had taken up nutriment from their surroundings to form granules (Mastung = good feeding).3
The mast cell granules were water soluble and showed metachromasia with certain basic dyes, where the cells of the tissue being examined acquired a colour other than that of the dye being used; for example, with toluidine blue stain mast cell granules stain red–purple. Blood basophils, described by Ehrlich in 1891, were also found to contain metachromatic granules, but whereas the more common tissue mast cell is born, lives and dies in the connective tissues, the comparatively rare basophil takes origin in the bone marrow and lives in the peripheral blood. As for their function, this became known as Ehrlich’s mast cell riddle.4
During the 60 years that followed Ehrlich’s discovery research on the mast cell was almost entirely histological. Tissue mast cells in mammals tend to occur in loose fibrillary connective tissue, especially around blood vessels, ducts and nerves, and underlying epithelial, serous and synovial membranes. With regard to tumours, mast cells often accumulate around established carcinomas in many species. Rarely, the mast cells themselves give rise to malignant growths, such mastocytomas occurring most commonly in dogs. Focal accumulations of mast cells are present in humans, especially in urticaria pigmentosa, a chronic urticaria that leaves brownish staining when inactive, first described clinically by Nettleship in 18695 and pathologically by Unna in his book in 1896.6
In 1937, interest in the mast cell was suddenly stirred by the claim that it is the site of formation or storage of the sulphated mucopolysaccharide heparin, the natural anticoagulant of the circulating blood.7 Heparin was so called because it was first isolated from dog liver, which is exceptionally rich in this glycosaminoglycan. Jorpes remarked in 1946: ‘There is no doubt whatsoever about the nature of the granular substance of the mast cells. It is heparin’.8 At the time, the feeling was that the well-known perivascular distribution of the mast cells was because they produced an anticoagulant that they poured into the circulating blood. The answer to Ehrlich’s riddle seemed to be solved.9
Mast cells – Riley studies
Some of this section of the mast cell story is compiled in Riley’s own words, as recounted in his autobiography Listening and Remembering.10
Two considerations led Riley to suspect that histamine, as well as heparin, might be present in mast cells. The first was the work carried out on peptone shock in the dog, where intravenous injection of peptone produces a state of shock and incoagulability of the blood due to histamine and heparin, respectively, both released principally from the liver in this species. Since heparin comes from mast cells, of which there are plenty in the dog’s liver, it seemed reasonable to suppose that histamine might also have its origin in the same cells. Secondly, the skin disease urticaria pigmentosa is histologically a ‘benign mastocytoma’, mild trauma to the skin being followed by the localised appearance of a grossly exaggerated ‘triple response’11 – visible evidence of a local release of histamine in the skin.12 Thus, both the general release of histamine into the blood stream of the dog and the local release of histamine into the skin of the human have this in common; that the ‘shock organ’ in each case is rich in mast cells.
It was already known that histamine was released in many injurious and hyper-reactive states, such as asthma, urticaria and certain allergies, and in 1937 the first of the antihistamines was introduced. As for histamine itself, no one yet knew where it was made, how it was stored or by what mechanism it was released. Valuable weapons were, however, coming to the aid of the problem in the shape of the histamine liberators. Among these was a toxic chemical called stilbamidine, which Riley knew was strongly fluorescent in ultraviolet light. He injected this into the tail vein of a rat and found that the mast cells around the small blood vessels in the peritoneum glowed transiently like neon street lights, before undergoing disruption with disappearance of the fluorescence. He wrote an excited letter to Nature, but a few days later his letter was returned.
Riley showed the letter to Alan Lendrum, the Professor of Pathology at Dundee, who remarked ‘H’m, perhaps it is a bit new for them’, and persuaded him to repeat the story as a short paper to the Scottish Society for Experimental Medicine in Dundee on 9 February 1952.13 At the meeting, the word ‘histamine’ caught the ear of Robert Hunter, the Chair of Pharmacology and Therapeutics, who had carried out some work on antihistamines and felt that he held proprietary rights in the field. Hunter sought out a pharmacologist called Geoffrey West (1916–90) at tea: “Come over here Geoff, and meet this ‘must’-cell fellow and see if you can’t dispose of him” (as recounted in Hunter‘s memoirs, which was typical of his humour and method). West had lingered over lunch and missed the paper, so Riley re-told his story, and in this way a most fruitful partnership sprang up between them. Here was the chance for Riley to work with a pharmacologist.
West had an open mind, and their tentative arrangement made over tea was that Riley would supply material of varied mast cell content and West would measure the amount of histamine in each, to see whether Riley’s predicted correlation with the mast cells did or did not exist. As simple as that. There followed a trip to the slaughterhouse, the addition of other tissues from the surgical laboratory, and placing a known weight of the tissue samples in small bottles of trichloroacetic acid to preserve any histamine that might be present. He then handed over the samples and a sealed envelope that contained Riley’s estimates to West, not to be opened until the calculations had been completed. It was the following Thursday that an excited West phoned to tell Riley that: “Well, you seem to have won the pools this week, you are ‘all correct’!”. Riley knew then that the mast cell was the main location of tissue histamine, although others were to need a lot more convincing.
On 17 May 1952, Riley delivered a presentation to the Physiological Society of Great Britain, of which West was a member. In it, he showed new data to support a common origin of histamine and heparin from mast cells in some normal animal tissues.14 The presentation seemed to receive a lukewarm reception, but at tea afterwards Riley was approached by none other than Sir Henry Dale, who had at one time worked with Ehrlich and had made extensive contributions to the study of histamine and anaphylaxis.15 Dale said: ‘I enjoyed your little talk in which, as I recall, you said that Ehrlich first clearly described and named the mast cells. I once worked with Ehrlich: he was an interesting fellow, full of stimulating ideas. My friend, Charlie Code in America, believes that histamine in the body is associated with the eosinophil cells, that is, with their basic granules. You imply that histamine may be carried in the acid granules of the mast cell. This is very curious. You must do some more work on this. You may be right; but we would like a little more evidence’. This was more than enough encouragement for Riley. He later came to know that Laennec was right when he said: ‘The first time they prick up their ears, the second registers and the third enters’. At his third Physiological Society meeting, mast cells were all the rage.
The paper that put Riley and West firmly in the spotlight was published the following year in the Journal of Physiology.16 They reported a strong positive correlation between the histamine and mast cell contents of a variety of normal and pathological tissues, with mast cells particularly numerous in ox and sheep liver capsules and ox pleura, these tissues contained considerably more histamine than in the underlying parenchyma (Figure 2). Adult organs rich in mast cells had more histamine than immature organs poor in mast cells. Storage of ox pleura and sheep liver resulted in a loss of extractable histamine, accompanied by the disappearance of tissue mast cells. Repeated painting of mice skin with a carcinogenic hydrocarbon increased both the histamine content and the mast cell population of the treated skin. Mast cell tumours contained exceptionally high concentrations of histamine. All the evidence suggested that tissue mast cells were rich in histamine.
Figure 2 Mast cells (prominent black dots) in ox lung, especially in pleura
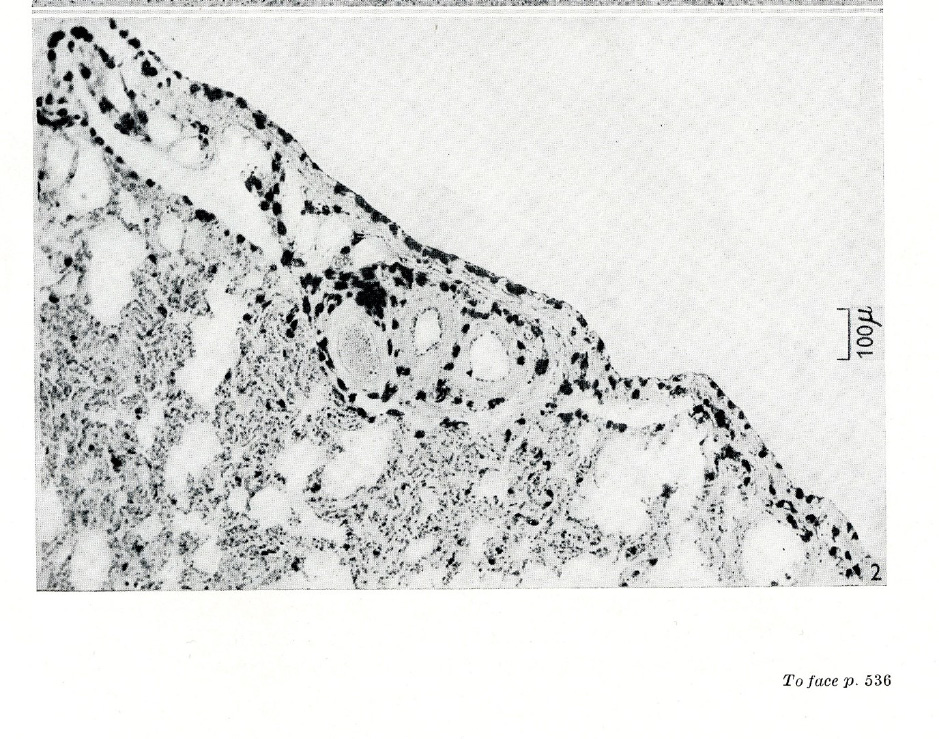
The significance of this striking positive correlation between the mast cell and histamine contents of normal tissues was greatly strengthened by the examination of pathological material abnormally rich in mast cells. Riley was able to examine tissue from several cases of human urticaria pigmentosa plus mast cell tumours in dogs, cats, cattle and mice, all demonstrating conclusively that an excessively high mast cell content is associated with a correspondingly high histamine value. One locally recruited golden cocker spaniel called Judy was found to have a record histamine level of 1,290 mg/g in a tumour recurrence (mast cells in dog mast cell tumours have 25–50 times the level of histamine of normal mast cells).17
In 1955, Riley and West were invited to contribute to a Ciba Symposium on Histamine in London, to be published as a ‘Festschrift’ to Sir Henry Dale on the occasion of his 80th birthday (Figure 3). Dale had chosen the subject as being one of the central themes of his own life as a research worker. The symposium ended with a dinner at which Riley was placed opposite Dale. At one point he enquired of Riley if there was yet any book on mast cells. When Riley replied that he knew of none, Dale smiled and suggested that Riley might write one. Emboldened with good food and wine, Riley replied that he would if Dale would write the foreword, to which Dale smiled and said he was getting good at forewords. In due course, Riley did write the book, published in 1959,18 and Dale did indeed write the foreword.
Figure 3 Histamine symposium for Sir Henry Dale 1955, Riley far right

In 1960, Riley was taken to Canada and America, and gave a Mayo Foundation lecture in a packed FC Mann Auditorium at Rochester. He was back in Canada in 1966, honoured for the international significance of his research work by being made a visiting professor at the University of Montreal, and was awarded the Claude Bernard Medal for medical achievement, complete with an elaborate celebratory cake (Figures 4 and 5). He was also elected a Fellow of the Royal Society of Edinburgh in 1968.
Figure 4 Teaching trainees at Montreal, 1966

Figure 5 Claude Bernard Professor celebratory cake, 1966

Close
Riley’s contribution is put into context in Hans Selye’s 1965 exhaustive review of the world literature on the mast cell, which cites 2,500 papers and acknowledges that the observations by Riley and West were seminal, praising their ‘elegant’ series of experiments.19 Furthermore, in a review of the mast cell in 2009, Beaven noted: ‘After a long period of largely descriptive studies which revealed little about the biological role of the mast cell, the field was galvanised in the 1950s by the recognition that the mast cell was the main repository of histamine and a key participant in anaphylactic reactions … The presence of histamine in mast cells was rigorously established in a notable series of studies by Riley and West in the period 1952-1956’.20 Beaven went on to say: ‘...recent research has now shown that the mast cell also plays a key role in innate and adaptive immune responses, autoimmune disease and possibly tissue homeostasis by virtue of its expression of a diverse array of receptors and biologically active products’. It sounded as though Ehrlich’s riddle still needed some thought to unravel.
In view of his original contributions, the University of St Andrews conferred upon Riley a Readership in Experimental Medicine in the 1960s, and he continued to contribute to the literature on mast cells, anaphylaxis, histamine/heparin and carcinogenesis, but his main research output had come in the 1950s. In recognition of his outstanding contribution to medicine, he was honoured in 2015 with a bronze plaque at Dundee’s Discovery Walk at Slessor Gardens on the Waterfront development, one of a series of plaques set into the walkway honouring the pioneering spirit of those whose scientific and social achievements have helped make Dundee and the wider world a better place.
Riley continued to work as a radiotherapist at DRI, but the move to the new Ninewells Hospital and Medical School in 1974 came just a bit late in his career, for he retired 2 years later at the age of 64 years. He had many interests outside of work; he wrote biographies on scientists such as Michael Faraday and wrote a Pelican original Introducing Biology; his autobiography was published posthumously.10 Tayside’s Medical History Museum is indebted to him for gathering together and preserving many historical artefacts and old equipment from the radiology and radiotherapy departments at DRI; these date back to its first radiologist, Dr George Pirie, one of the Radiology Martyrs who lost their lives to the damaging effects of X-rays who are celebrated on the 1936 Martyrs’ Memorial in Hamburg. Pirie is also honoured with a plaque at Dundee’s Discovery Walk.
In 1974 Riley developed the first symptoms of cerebrovascular disease and he retired soon after. In typical fashion he completed his autobiography. He enjoyed rambles in the countryside around Dundee with his wife Marina, involvement with his grandchildren and holiday trips. On one such trip to Yorkshire he suffered his first stroke, and he passed away in 1985.
Acknowledgements
I wish to acknowledge the help given to me by the Riley family in the preparation of this manuscript. They have kindly consented to the use of extracts from Dr Riley’s autobiography and photographs from the family collection.
References
1 Recklinghausen F von. Über Eiter und Bindegewebskörperchen [in German]. Virchows Arch 1863; 28: 157–97.
2 Waldeyer W. Über Bindegewebszellen [in German]. Arch mikrosk Anat 1875; 11: 176–94.
3 Ehrlich P. Beiträge zur Theorie und Praxis der histologischen Färbung [in German]. 1878; Thesis Leipzig University.
4 Riley J. The riddle of the mast cells; a tribute to Paul Ehrlich. Lancet 1954; 266: 841–3.
5 Nettleship E. Rare forms of urticaria 1 chronic urticaria, leaving brown stains: nearly two years duration. Br Med J 1869; II: 323.
6 Unna PG. The Histopathology of the Diseases of the Skin. Edinburgh: Clay New York Macmillan; 1896.
7 Holmgren H, Wilander O. Beitrag zur Kenntnis der Chemie und Funktion der Ehrlichschen Mastzellen [in German]. Ztschr mikr-anat Forsch 1937; 42: 242–78.
8 Jorpes JE. Heparin in the Treatment of Thrombosis. 2nd Edition. London: OUP; 1946. p. 60.
9 Riley JF. The Mast Cells. Edinburgh and London: E & S Livingstone Ltd; 1959. p. 29.
10 Riley JF. Listening and Remembering, Memoirs of a Settle Boy. Settle: Lamberts Print and Design; 2005.
11 Lewis T. The Blood Vessels of the Human Skin and Their Responses. London: Shaw; 1927.
12 Dale HH. Some chemical factors in the control of the circulation. Lecture II. Local vasodilator reactions – histamine. Lancet 1929; I: 1233.
13 Riley JF. Proc Scot Soc Exp Med Dundee meeting. 9 February 1952.
14 Riley JF, West GB. Histamine in tissue mast cells. Proc Physiol Soc J Physiol 1952; 117: 72.
15 Riley JF. Histamine and Sir Henry Dale. Br Med J 1965; 1488–90.
16 Riley JF, West GB. The presence of histamine in tissue mast cells. J Physiol 1953; 120: 528–37.
17 Northrup N. Mast cell tumors in dogs and cats (Proceedings). 2008. http://veterinarycalendar.dvm360.com/mast-cell-tumors-dogs-and-cats-proceedings (accessed 13/02/19).
18 Riley JF. The Mast Cells. Edinburgh and London: E & S Livingstone Ltd; 1959.
19 Selye H. The Mast Cells. London: Butterworth Inc.; 1965. p. 4.
20 Beaven MA. Our perception of the mast cell from Paul Ehrlich to now. Eur J Immunol 2009; 39: 11–25.